Paul, MN), and the CARTO ® 3 mapping platform was used along with the CARTOSOUND ® module, which enabled integration of the ICE images with the 3D mapping images ( Figure). Three-dimensional (3D) mapping was performed using a 7F variable-curve Lasso catheter (Biosense Webster, Diamond Bar, CA) inserted through an SL1 sheath (St. A 10F SOUNDSTAR ® (Biosense Webster, Diamond Bar, CA) intracardiac echocardiogram (ICE) catheter was placed in the right atrium for anatomic mapping of the left atrium, left atrial appendage, and pulmonary veins, and under ICE guidance a double transseptal puncture was performed using a Brockenbrough needle assembly. A commercially available nondeflectable transesophageal temperature probe (Level 1 Acoustascope ® with temperature sensor ES400-18 Smiths Medical ASD, Inc, Rockland, MA) was inserted to monitor luminal esophageal temperature (LET). Repeat TEE showed no residual thrombus in the left atrial appendage. The night prior to the procedure, rivaroxaban was discontinued and a weight-based continuous infusion of unfractionated heparin was started periprocedurally. A transesophageal echocardiogram (TEE) with echo-contrast performed 2 months prior demonstrated a thrombus within the left atrial appendage, and he was prescribed rivaroxaban at a renal-adjusted dose of 15 mg daily. Clinicians need to be aware of and recognize this complication, quickly distinguish it from other potentially life-threatening conditions such as esophageal perforation or bowel obstruction, and institute an appropriate treatment plan.Ī 56-year-old man with hypertension, type 2 diabetes mellitus, hyperlipidemia, obstructive sleep apnea, chronic kidney disease, and diastolic heart failure was admitted for an elective catheter ablation for recurrent paroxysmal AF. One of these complications is periesophageal vagal nerve injury, which leads to acute onset of upper GI symptoms that typically develop within hours after ablation. In recent years there have been several reports of other complications that affect the upper GI tract following catheter ablation for AF. However, atrioesophageal fistulae can lead to potentially life-threatening sequelae including catastrophic bleeding, septicemia, cerebrovascular accidents, and air embolism, and carry a mortality rate exceeding 80%.
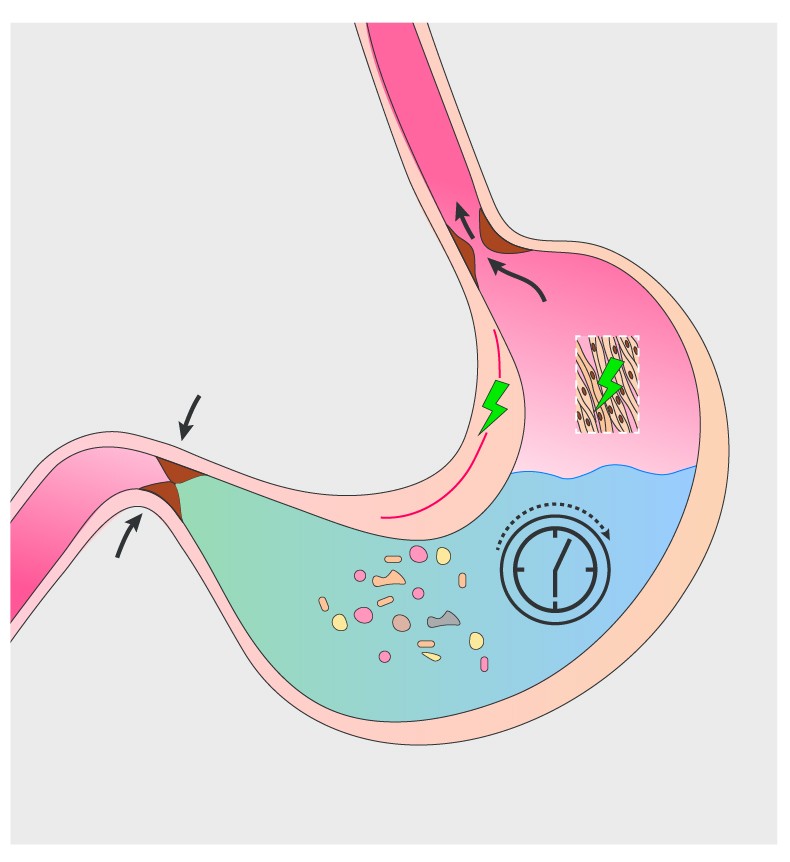
The most serious GI complication after catheter ablation is formation of an atrioesophageal fistula, which has a very low incidence (0.03%-0.1% of cases). 6 Gastrointestinal (GI) complications following catheter ablation for AF are exceedingly rare. The majority of the complications were vascular in nature with an incidence of 1.4%. A recently published retrospective analysis of AF catheter ablation (performed in 83,236 patients enrolled in a total of 192 published clinical trials) reported an overall periprocedural complication rate of 2.9%.
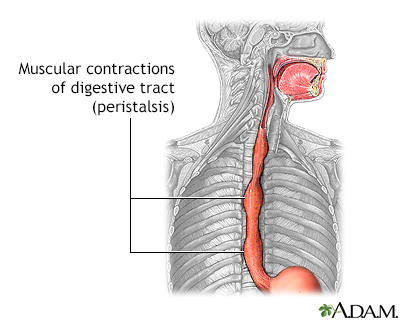
5Ĭatheter ablation for AF is widely regarded as a safe procedure. 3, 4 Catheter ablation has garnered a class I recommendation for patients with symptomatic paroxysmal AF who are refractory or intolerant to at least one class I or III antiarrhythmic medication, and has a class IIa recommendation as a reasonable initial rhythm control strategy in the 2014 guidelines published by the American College of Cardiology/American Heart Association/Heart Rhythm Society. 1, 2 Recent clinical trials show that catheter ablation of atrial fibrillation reduces the risk of recurrence of symptomatic AF, atrial flutter, or atrial tachycardia, and may also reduce subsequent hospitalizations and improve quality of life compared to antiarrhythmic drug therapy. Percutaneous catheter ablation is an established rhythm control strategy for the treatment of atrial fibrillation (AF).

